A universal influenza vaccine with the potential to be longer lasting and more effective than commercially available vaccines is destined for human clinical trials, thanks to a $17.9 million grant from the National Institute of Allergy and Infectious Diseases.
The grant was awarded to Versatope Therapeutics, a biotechnology startup founded by a team including David Putnam, professor of biomedical engineering, and Matt DeLisa, the William L. Lewis Professor of Chemical and Biomolecular Engineering. Putnam and DeLisa developed the vaccine at Cornell and published a study in 2017 detailing its potential.
The universal vaccine is engineered differently from commercially available vaccines, which are not always effective because they protect against a small number of influenza strains. Health officials do their best to match vaccines with the strains, but proteins in the virus can mutate as they spread.
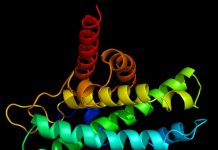
The vaccine developed at Cornell focuses on a portion of the virus – the Matrix-2 protein – that remains relatively constant from strain to strain. To properly train the body’s immune system to protect against influenza, the Matrix-2 protein is displayed on the surface of bacterial outer membrane vesicles, where it is prominently presented to the immune system upon delivery of the vesicle-based vaccine.
The vaccine is designed to protect people for a long time, making it like a tetanus shot where you have a booster every few years, not like the traditional influenza vaccine that needs to be given annually.”
David Putnam, professor of biomedical engineering, Cornell University
Versatope Therapeutics said in a statement that the grant “will support manufacturing, stability and human clinical studies to demonstrate safety and tolerability in healthy volunteers.” Putnam said the funding will carry the company through Phase I clinical trials, which could begin as early as 2021.
The universal vaccine performed well during clinical trials in mice, conducted by Gary Whittaker, professor of virology in the College of Veterinary Medicine. Mice that received the vaccine developed an immune response to the virus twice as fast as they did with commercially available vaccines, and carried the immune response for six months, the average lifespan of the animal.
In collaboration with the Centers for Disease Control and Prevention, the vaccine also was shown to be effective in ferrets. Efficacy in ferrets correlates well with the vaccine’s potential efficacy in humans, according to the research team.
“Dave and I have been collaborating on this theme for the better part of a decade,” DeLisa said, “so it’s now very rewarding to see the technology moving from our laboratories and into the clinic, where it will have an opportunity to impact such an important health issue.”