 insights from industryPatrick SwanCheif Operating OfficerGold Biotechnology
insights from industryPatrick SwanCheif Operating OfficerGold BiotechnologyAn interview with Patrick Swan, COO of Gold Biotechnology, discussing the effects of mycoplasma contamination on cell cultures and the development of rapid detection kits that provide answers in just thirty minutes.
What impact does mycoplasma have on cell cultures and experimental results?
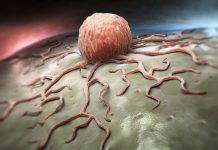
Mycoplasma can have a drastic effect on cells and cell cultures, to the point where a contaminated culture may not work the way that it is supposed to, as it may not metabolize things correctly or grow correctly. Such a small thing can have substantial effects.
All aspects of self-physiology can be impacted. For example, competition can mean that your cells are smaller than they should be.
Mycoplasma contamination prevents you from obtaining the standard of experimental results that you are supposed to have. There has been a new variable introduced, and so the results are not valid anymore. This causes a big problem when it comes to reviewing experimental results and not being able to replicate your published results.
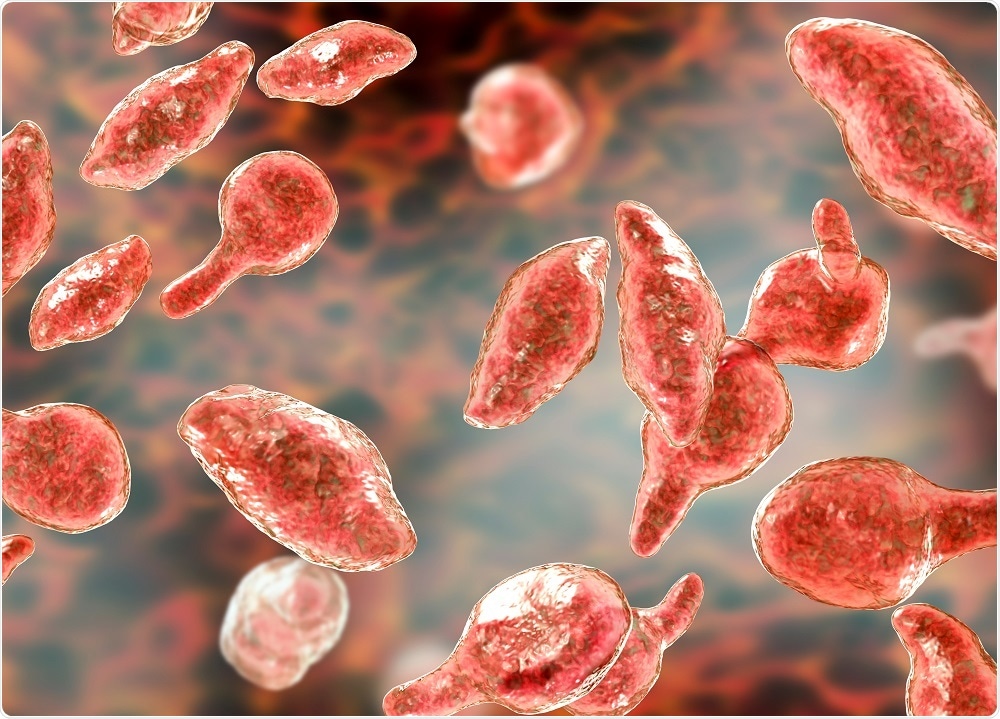 Image Credit: Kateryna Kon / Shutterstock.com
Image Credit: Kateryna Kon / Shutterstock.com
What techniques have traditionally been used to detect mycoplasma in cell cultures?
There are a lot of different techniques, the standard being tissue culture. The problem with this is that while it is very sensitive and accurate, it takes at least 28 days. It is also time-consuming, so if you are pressed for time, this is not a suitable method.
Bioluminescence is another way to detect mycoplasma. However, the detection sensitivity is just not up to par with something that is qPCR based. There are also other types of tests, such as Elisa tests.
With all the methods, you have to be consistent with your testing methodology, and this can be difficult. Furthermore, the sensitivity on many of these commercially available kits is not as high as it could be. Therefore, you might have mycoplasmal contamination in your cell line that you do not know about immediately; unfortunately, it can remain undetected until the end.
Why are new techniques desperately needed for the detection of mycoplasma?
The main reason is the length of time that it currently takes to detect mycoplasma contamination. After culturing, you then have to carry out DNA extraction, which increases the risk of human error. When carrying out PCR, you are dealing with incredibly small volumes. If something goes slightly wrong, your result is going to be affected.
In addition, sometimes PCR does not work, and there is no explanation for this. That can be detrimental because if you do not have the right controls set or something is out of place, you may get a negative which should be a positive and vice versa. The new methodologies should be simpler by automating this process.
 Image Credit: angellodeco / Shutterstock.com
Image Credit: angellodeco / Shutterstock.com
If mycoplasma is detected early, can the cell line be saved?
In theory, yes, but it is neither simple nor easy. Getting rid of mycoplasma after detection is difficult. There are commercially available kits to help get rid of mycoplasma, but they aren’t 100% effective. They may not completely remove the contamination from the lab itself, or may only treat the cell line, and so the chances of reinfection can be high. The odds are not in your favor.
How are the certus mycoplasma detection kits filling this gap?
Our mycoplasma detection kits rely on isothermal amplification and use a similar mechanism to qPCR. A sample from any cell media is added to primers and amplified in a real-time qPCR machine, with a melt curve analysis carried out at the end.
There is built-in positive and negative control, which guarantees the right results in that respect. It has been shown to be repeatable and is very fast, with a hands-on time of five minutes. In total, the process takes around 20-30 minutes.
There are two kits: the standard and the advanced. Our advanced kit, which is the higher end of the two, is one of the most sensitive tests on the market. It can detect down to one CFU per mil of mycoplasma, which is an incredible sensitivity. Both kits are currently available in the US.
How does the sensitivity compare to traditional techniques?
The sensitivity is comparable to cell culture. However, it is far quicker. It is far more sensitive than bioluminescence. The issue with some bioluminescence kits is that you can get false negatives, which can be wrongly reassuring. It can make a devised thesis completely invalid.
You offer two kits for mycoplasma detection. What’s the difference between the two, and when should each one be used?
If you are a standard laboratory, then the standard kit is going to make sense. The advanced kit is useful in places where it is imperative to make sure that absolutely no mycoplasma is present, and this is tested for consistently. This includes cell banks and CROs, or anywhere where they are delivering a product that is certifiably mycoplasma free.
This kit offers species detection too. There are three additional species detected by the advanced kit, which are approved by the European and American pharmacopeia.
Furthermore, the standard kit will only test supernatants, whereas the advanced kit can test cell suspensions or supernatants.
Are the kits approved for use by the United States Pharmacopeia and European Pharmacopeia?
They are not approved yet, but we are working on it. We are taking steps to get a GMP certification for production, and hopefully, from that, we will obtain pharmacological society approval. The kits meet testing standards, but we are still going through the last official steps.
Do you have any advice for scientists struggling with mycoplasma contamination?
Mycoplasma contamination is very difficult. If a lab is consistently having mycoplasma contamination issues, everything needs to be taken back to basics and all the workers’ techniques checked.
There are different measures that can be taken in the lab to decontaminate surfaces and make sure that incubators are decontaminated regularly and correctly. If cells are being moved between buildings or rooms during the procedure, there are products designed to keep them safe from exposure to potential contamination.
Illness is also an important contamination factor – no one should go into the lab if they are ill. For example, take pneumonia, which is caused by mycoplasma. Coughing or sneezing in the lab while having pneumonia could cause the spread of mycoplasma. People should not be working in the lab if they are sick.
 Image Credit: ArtPanupat / Shutterstock.com
Image Credit: ArtPanupat / Shutterstock.com
These detection kits are a new innovation that could help millions of scientists around the world. What’s next for the company?
Gold Bio has been creating products for 35 years now. We are continuing to add new products to the suit and hope to build an exhaustive culture line. We have new products for bacterial research; some to do with cell culture and others pertaining to DNA and protein research, along with many other important life science categories. Our aim is to keep growing as the market and the research itself grows.
Where can our readers find more information?
certus QC – mycoplasma detection kits
About Patrick Swan
 Patrick Swan is currently the Chief Operating Officer of Gold Biotechnology, and has been with the company for over 10 years. After earning bachelor’s degrees in molecular biology and psychology from Truman State University, GoldBio hired him initially to be a summer intern.
Patrick Swan is currently the Chief Operating Officer of Gold Biotechnology, and has been with the company for over 10 years. After earning bachelor’s degrees in molecular biology and psychology from Truman State University, GoldBio hired him initially to be a summer intern.
During his time, he has helped GoldBio grow into an internationally renowned company, and he is truly passionate about the company’s mission of providing researchers with the highest quality products at reasonable prices. Patrick is currently finishing an MBA from the Olin School of Business. In his free time, he enjoys spending as much time as he can with his wife and two young children, usually doing something outdoorsy.
Sponsored Content Policy: News-Medical.net publishes articles and related content that may be derived from sources where we have existing commercial relationships, provided such content adds value to the core editorial ethos of News-Medical.Net which is to educate and inform site visitors interested in medical research, science, medical devices and treatments.